Abstract
Objectives
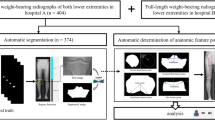
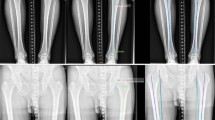
Accurate assessment of knee alignment and leg length discrepancy is currently measured manually from standing long-leg radiographs (LLR), a process that is both time consuming and poorly reproducible. The aim was to assess the performance of a commercial available AI software by comparing its outputs with manually performed measurements.
Materials and methods
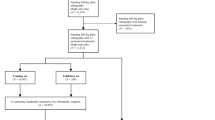
The AI was trained on over 15,000 radiographs to measure various clinical angles and lengths from LLRs. We performed a retrospective single-center analysis on 295 LLRs obtained between 2015 and 2020 from male and female patients over 18 years. AI and expert measurements were performed independently. Kellgren-Lawrence score and reading time were assessed. All measurements were compared and non-inferiority, mean-absolute-deviation (sMAD), and intra-class-correlation (ICC) were calculated.
Results
A total of 295 LLRs from 284 patients (mean age, 65 years (18; 90); 97 (34.2%) men) were analyzed. The AI model produces outputs on 98.0% of the LLRs. Manually annotations were considered as 100% accurate. For each measurement, its divergence was calculated, resulting in an overall accuracy of 89.2% when comparing the AI outputs to the manually measured. AI vs. mean observer revealed an sMAD between 0.39 and 2.19° for angles and 1.45–5.00 mm for lengths. AI showed good reliability in all lengths and angles (ICC ≥ 0.87). Non-inferiority comparing AI to the mean observer revealed an equivalence-index (γ) between 0.54 and 3.03° for angles and − 0.70–1.95 mm for lengths. On average, AI was 130 s faster than clinicians.
Conclusion
Automated measurements of knee alignment and length measurements produced with an AI tool result in reproducible, accurate measures with a time savings compared to manually acquired measurements.






Similar content being viewed by others
References
Skyttä ET, Lohman M, Tallroth K, Remes V. Comparison of standard anteroposterior knee and hip-to-ankle radiographs in determining the lower limb and implant alignment after total knee arthroplasty. Scand J Surg. 2009 [cited 2021 Jun 8];98:250–3. Available from: http://journals.sagepub.com/doi/10.1177/145749690909800411
Zheng Q, Shellikeri S, Huang H, Hwang M, Sze RW. Deep learning measurement of leg length discrepancy in children based on radiographs. Radiology. 2020 [cited 2021 Jun 8];296:152–8. Available from: http://pubs.rsna.org/doi/10.1148/radiol.2020192003
Hankemeier S, Gosling T, Richter M, Hufner T, Hochhausen C, Krettek C. Computer-assisted analysis of lower limb geometry: higher intraobserver reliability compared to conventional method. Comput Aided Surg. 2006 [cited 2021 Jun 8];11:81–6. Available from: http://www.tandfonline.com/doi/full/10.3109/10929080600628985
Schmidt G, Altman G, Dougherty J, DeMeo P. Reproducibility and reliability of the anatomic axis of the lower extremity. J Knee Surg. 2010 [cited 2020 Sep 8];17:140–3. Available from: http://www.thieme-connect.de/DOI/DOI?10.1055/s-0030-1248212
McDaniel G, Mitchell KL, Charles C, Kraus VB. A comparison of five approaches to measurement of anatomic knee alignment from radiographs. Osteoarthr Cartil. NIH Public Access; 2010 [cited 2020 Sep 8];18:273–7. Available from:/pmc/articles/PMC2818371/?report=abstract
Boese CK, Wilhelm S, Haneder S, Lechler P, Eysel P, Bredow J. Influence of calibration on digital templating of hip arthroplasty. Int Orthop. 2019 [cited 2021 Jun 8];43:1799–805. Available from: http://link.springer.com/10.1007/s00264-018-4120-7
Franken M, Grimm B, Heyligers I. A comparison of four systems for calibration when templating for total hip replacement with digital radiography. J Bone Joint Surg Br. 2010 [cited 2021 Jun 8];92-B:136–41. Available from: http://online.boneandjoint.org.uk/doi/10.1302/0301-620X.92B1.22257
Vaishya R, Vijay V, Birla VP, Agarwal AK. Inter-observer variability and its correlation to experience in measurement of lower limb mechanical axis on long leg radiographs. J Clin Orthop Trauma. 2016 [cited 2021 Jun 8];7:260–4. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0976566216300613
Duron L, Ducarouge A, Gillibert A, Lainé J, Allouche C, Cherel N, et al. Assessment of an AI aid in detection of adult appendicular skeletal fractures by emergency physicians and radiologists: a multicenter cross-sectional diagnostic study. Radiology. 2021 [cited 2021 Aug 2];203886. Available from: http://pubs.rsna.org/doi/10.1148/radiol.2021203886
Bini SA. Artificial intelligence, machine learning, deep learning, and cognitive computing: what do these terms mean and how will they impact health care? J Arthroplasty. 2018 [cited 2021 Aug 2];33:2358–61. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0883540318302158
Rouzrokh P, Ramazanian T, Wyles CC, Philbrick KA, Cai JC, Taunton MJ, et al. Deep learning artificial intelligence model for assessment of hip dislocation risk following primary total hip arthroplasty from postoperative radiographs. J Arthroplasty. 2021 [cited 2021 Aug 2];36:2197–2203.e3. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0883540321001674
Ramkumar PN, Karnuta JM, Navarro SM, Haeberle HS, Scuderi GR, Mont MA, et al. Deep learning preoperatively predicts value metrics for primary total knee arthroplasty: development and validation of an artificial neural network model. J Arthroplasty. 2019 [cited 2021 Aug 2];34:2220–2227.e1. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0883540319305170
Krogue JD, Cheng K V., Hwang KM, Toogood P, Meinberg EG, Geiger EJ, et al. Automatic hip fracture identification and functional subclassification with deep learning. Radiol Artif Intell. 2020 [cited 2021 Aug 2];2:e190023. Available from: http://pubs.rsna.org/doi/10.1148/ryai.2020190023
American college of Radiology. Image Interpretive. 2021 [cited 2021 Aug 2]. Available from: https://www.acrdsi.org/DSI-Services/Define-AI#int
Schock J, Truhn D, Abrar DB, Merhof D, Conrad S, Post M, et al. Automated analysis of alignment in long-leg radiographs using a fully automated support system based on artificial intelligence. Radiol Artif Intell. 2020 [cited 2021 Jun 8];e200198. Available from: http://pubs.rsna.org/doi/10.1148/ryai.2020200198
Nehrer S, Ljuhar R, Steindl P, Simon R, Maurer D, Ljuhar D, et al. Automated knee osteoarthritis assessment increases physicians’ agreement rate and accuracy: data from the osteoarthritis initiative. Cartilage. 2019 [cited 2021 Jun 10];194760351988879. Available from: http://journals.sagepub.com/doi/10.1177/1947603519888793
Paley D. Principles of deformity correction. Princ Deform Correct. Berlin, Heidelberg: Springer Berlin Heidelberg; 2002 [cited 2021 Jun 10]. p. 19–30. Available from: http://link.springer.com/10.1007/978-3-642-59373-4
Waldt, Simone, Matthias Eiber and KW. Messverfahren und Klassifikationen in der muskuloskelettalen Radiologie. 2nd ed. Verlag GT, editor. Stuttgart; 2017.
Knutson GA. Anatomic and functional leg-length inequality: a review and recommendation for clinical decision-making. Part I, anatomic leg-length inequality: prevalence, magnitude, effects and clinical significance. Chiropr Osteopat. 2005 [cited 2021 Jun 10];13:11. Available from: https://chiromt.biomedcentral.com/articles/10.1186/1746-1340-13-11
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016 [cited 2021 Jun 10];15:155–63. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1556370716000158
Obuchowski NA, Subhas N, Schoenhagen P. Testing for interchangeability of imaging tests. Acad Radiol. 2014 [cited 2021 Jun 10];21:1483–9. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1076633214002499
Schmale GA, Bayomy AF, O’Brien AO, Bompadre V. The reliability of full-length lower limb radiographic alignment measurements in skeletally immature youth. J Child Orthop. 2019 [cited 2021 Jun 11];13:67–72. Available from: https://online.boneandjoint.org.uk/doi/10.1302/1863-2548.13.180087
J. M. Mellado1, I. Quintana, N. Yanguas, J. Salceda Artola, I. Sanmartin RMCC. Normal anatomy and variations of the proximal femur: a reappraisal with 64-slice MDCT. Eur Congr Radiol. 2014 [cited 2021 Jun 11]; Available from: https://doi.org/10.1594/ecr2014/C-1825
Kiener M. Artificial intelligence in medicine and the disclosure of risks. AI Soc. 2020 [cited 2021 Jun 11]; Available from: http://link.springer.com/10.1007/s00146-020-01085-w
Holme TJ, Henckel J, Hartshorn K, Cobb JP, Hart AJ. Computed tomography scanogram compared to long leg radiograph for determining axial knee alignment. Acta Orthop. 2015 [cited 2021 Jun 11];86:440–3. Available from: http://www.tandfonline.com/doi/full/10.3109/17453674.2014.1003488
Babazadeh S, Dowsey MM, Bingham RJ, Ek ET, Stoney JD, Choong PFM. The long leg radiograph is a reliable method of assessing alignment when compared to computer-assisted navigation and computer tomography. Knee. 2013 [cited 2021 Jun 11];20:242–9. Available from: http://www.ncbi.nlm.nih.gov/pubmed/22892197
Sled EA, Sheehy LM, Felson DT, Costigan PA, Lam M, Cooke TD V. Reliability of lower limb alignment measures using an established landmark-based method with a customized computer software program. Rheumatol Int. 2011 [cited 2021 Jun 11];31:71–7. Available from: http://link.springer.com/10.1007/s00296-009-1236-5
Bowman A, Shunmugam M, Watts AR, Bramwell DC, Wilson C, Krishnan J. Inter-observer and intra-observer reliability of mechanical axis alignment before and after total knee arthroplasty using long leg radiographs. Knee. Elsevier B.V.; 2016;23:203–8.
Rauh MA, Boyle J, Phillips MJ, Mihalko WM, Krackow KA, Bayers-Thering M. Reliability of measuring long-standing lower extremity radiographs. Orthopedics. 2007 [cited 2021 Jun 11];30:299–303. Available from: https://www.healio.com/orthopedics/knee/journals/ortho/2007-4-30-4/%7B5932395d-5d73-42d2-a5a3-5dd3c9f90e6d%7D/reliability-of-measuring-long-standing-lower-extremity-radiographs
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Although none of the authors has received or will receive benefits for personal or professional use from a commercial party related directly or indirectly to the subject of this article, benefits have been or will be received but will be directed solely to a research fund, foundation, educational institution, or other non-profit organization with which one or more of the authors are associated.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Simon, S., Schwarz, G.M., Aichmair, A. et al. Fully automated deep learning for knee alignment assessment in lower extremity radiographs: a cross-sectional diagnostic study. Skeletal Radiol 51, 1249–1259 (2022). https://doi.org/10.1007/s00256-021-03948-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03948-9